Become an Incathlab member and receive full access to its content!
Registration Login
Operators and Faculty

Prof. Piero Montorsi
Director of II Unit Interventional Cardiology, Centro Cardiologico Monzino, Italy.

Prof. Gioachino Coppi
Chief of cardiac and vascular disease department, A.O. University and AUSL Modena, Italy.

Prof. Alberto Cremonesi
Chief of cardio-vascular department Maria Cecilia Hospital and President at Italian Society of Invasive and Interventional Cardiology SICI-GISE, Italy.

Dr. Stefano Galli
Interventional cardiologist, II Unit Interventional Cardiology, Centro Cardiologico Monzino, Milan, Italy.

Dr. Eugenio Stabile
Interventional Cardiologist, Casa di Cura Montevergine, Mercogliano, Italy.
&

Dr. L.Caputi
Neurologist c/o Department of Cerebrovascular Diseases, Neurological Institute C. Besta, Italy
Program
04 pm - 04.15 pm
Different protection devices during CAS
One, No one, and one hundred Thousand*
Prof. P. Montrosi
04.15 pm - 06 pm
Live case
Operators: Prof. P. Montorsi - Dr. E. Stabile
Dr. L.Caputi (neurologist) will perform intra procedural TCD assessment
06 pm - 07 pm
Discussion & Conclusion
Answer to chat questions
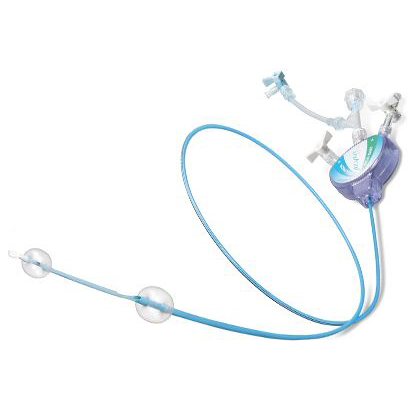
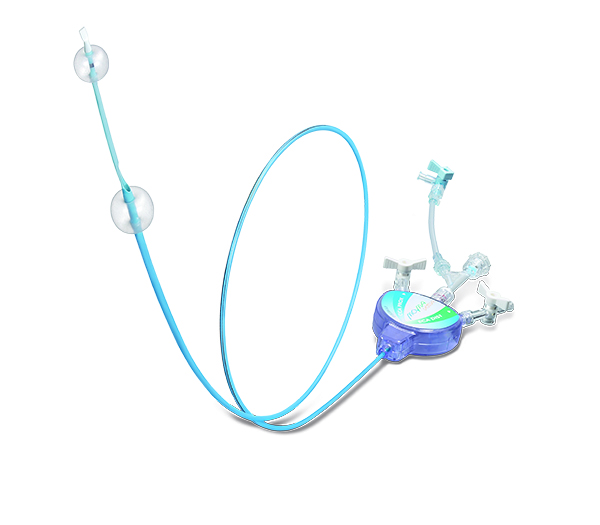
MOMA device
Angiographies
| Baseline Angiography RICA (RAO 45°) | Occlusion test | Final result |
Produced in collabaration with
Last update : 2021-06-09
Tailored protection device for selected patients during CAS: The role of proximal protection systems
(Live from Centro Cardiologico Monzino, Italy)
Operators and Faculty
- Prof. Piero Montorsi
Director of II Unit Interventional Cardiology, Centro Cardiologico Monzino, Italy.
- Prof. Gioachino Coppi
Chief of cardiac and vascular disease department, A.O. University and AUSL Modena, Italy.
- Prof. Alberto Cremonesi
Chief of cardio-vascular department Maria Cecilia Hospital and President at Italian Society of Invasive and Interventional Cardiology SICI-GISE, Italy.
- Dr. Stefano Galli
Interventional cardiologist, II Unit Interventional Cardiology, Centro Cardiologico Monzino, Milan, Italy.
- Dr. Eugenio Stabile
Interventional Cardiologist, Casa di Cura Montevergine, Mercogliano, Italy.
- Dr. Luigi Caputi
Neurologist c/o Department of Cerebrovascular Diseases, Neurological Institute C. Besta, Italy
Different protection devices during CAS: One, No one, and one hundred Thousand
By Prof. P. Montorsi
Hello! Welcome to Milan, Centro Cardiologico Monzino. It’s 4PM in the afternoon. My name is Piero Montorsi. Close to me is Stefano Galli and Eugenio Stabile. This is a very good important team that will show you an interesting case of carotid stenting with proximal protection. The patient is all ready of course on the table and has been prepped. Everything is in the right place. And I'm going to show you some slides, before starting the case, talking about proximal protection. Very quickly -- 10 minutes or even less…
SHOULD WE PROTECT THE BRAIN?
The first question is: "Should we protect the brain?" The answer is yes. There is no actually randomized controlled study that has seen the difference without or with distal protection.
This is a very old slide that tell us that if you protect the brain, you can reduce the combined endpoint, major stroke, and minor stroke. So there is some evidence, even if not randomized, that protection is better.
TYPES OF AVAILABLE CEREBRAL PROTECTION DEVICE
1. Distal cerebral protection - with a distal single balloon, filters, or FiberNet (something in between the first two)
2. Proximal protection -- Flow arrest and Flow reversal
This is just a cartoon to show you what it means.
1. Distal balloon - you already know, it occludes only the ICA.
2. Distal filter - your most used device.
3. Distal filter with FiberNet - is a special distal filter. We'll talk a little bit about it in a few seconds.
4. Proximal protection with flow arrest
5. Proximal protection with flow reversal
ADVANTAGES AND DISADVANTAGES OF THE DISTAL BALLOON
The Percusor is the commercial name.
Advantages
1. Complete protection of the distal ICA
Actually, you can achieve complete protection of the distal ICA with a distal balloon, apart from the crossing of the lesion that is a totally unprotected step.
2. Low crossing profile (0.036" up to 6mm balloon diameter)
3. Highly flexible
4 One size fits all (3-6mm)
Disadvantages
1. Blood flow interruption can lead to intolerance even in very, very low digits
2. Lesion crossing unprotected
3. No angio guidance - you should use landmarks
4. Potential ICA spasm/dissection
5. Potential embolization through ECA
6. Difficulties to cross tight and angulated lesions
This is just an example of a balloon that occluded the distal ICA. And if you inject contrast of anyway, the blood flow coming from the common may embolize some material during intervention through the external via the ophthalmic artery. It's rare but it can occur.
FILTERS
So many filters are available in the clinical arena. You should place the filter down in the distal ICA before it enters the skull. What are the advantages and disadvantages?
Advantages
1. Intuitive approach - We learn from other district?? [00:04:32.09]
2. Easy to use (in easy case)
3. Preserve ICA flow - so no panic. You can see the flow blowing and there is less emotional impact for the operator.
4. Angiographic lesion control during the entire procedure
5. Do not significantly prolong procedural time (in easy and experience hands)
Disadvantages
1. Larger profile, less flexible, less torquability
2. May need pre-predilation (10-20%) - if the stenosis is quite severe
3. May need "buddy wire" en toto distal ICA
4. May cause dissection/spasm of distal ICA
5. May detach from wire and embolize
6. May get stuck in stent
However, the most important disadvantages are:
7. Wire/filter crossing of the stenosis is unprotected
8. Lack of capture of particles smaller than filter pores (<80-100 microns)
9. Filter suboptimal wall apposition leading to particles passage between the filter basket and the vessel wall - especially if the distal ICA is quite tortuous
10. "Squeezing" of the captured material during filter withdrawal.
Nevertheless, this device is currently use in 80-85% of CAS procedures all over the world.
COMPLICATIONS WITH FILTERS
Is there any complication with filters? Complications detract many operators to use them, especially the neuroradiologists.
This is an always quoted paper by Reimers, B. (Am J Med 2004; 116:217)
| Protection device-related complications
| 5/640 (0.8%) |
| Dissection
| 4/640 (0.6%) |
| Filter entrapment
| 1/640 (0.15%) |
| Flow-limiting distal ICA spasm
| 27/640 (4.2%) |
| Flow impairment (filter obstruction)
| 51/640 (7.9%) |
There is no major complication.
DISTAL CEREBRAL PROTECTION (The FiberNet EPS)
The FiberNet is in between the single balloon and a filter. It is a low profile 0.014" guidewire-based system with a unique filter made by PTE fibers with 3-dimensional design (2.4F crossing profile). When it is open, it conforms to irregular vessel anatomy to effectively move fluid (so the blood flow is preserved). You can see the blood flow flowing. It efficiently captures and contains emboli as small as 40 microns -- smaller than the filters. The filter is recaptured by a dedicated 5F rapid exchange retrieval/aspiration catheter.
Here is an example of a stenosis. The filter is in the distal ICA. You can see the two markers. When you deploy the filter from the un-deployed to the deployed phase, the two markers get together ensuring that the filter is well open.
Distal Cerebral Protection with the FiberNet-EPS: The EPIC trial
By Myla S. CCI 2010; 75:817
The EPIC trial told us that the results are quite good, with a 3% composite endpoint, and 2% stroke and death-related. It’s quite good.
Are filters, single balloon, or FiberNet effective? These are high surgical risk patients (the most difficult subset of patients) results over the time. You can see that over the time, the filters do better and better -- as low as 2.5 with the FiberNet.
PROXIMAL PROTECTION: A different concept
The concept was if you inflate a balloon in the common carotid artery (see the right part of the slide) and you inflate a balloon in the external carotid artery, you will reverse the blood flow from the brain to the aorta. So you will be able to do carotid stenting, do predilation -- do whatever you want -- and you will be sure that no debris will flow to the brain because of the inverted flow. This is because of the back pressure when you invert the blood flow ensuring that the flow is going now from the brain to the aorta. You of course need a very collateralized hemisphere if you want to use the MOMA protection.
TYPES OF PROXIMAL PROTECTION
Three systems are in the market:
1. The MOMA System is a flow arrest.
2. The Gore System is a flow reversal. Differently from the MOMA, there is a fistula that is created by the operator from the arterial to the venous side allowing blood flow to flow during the procedure, making a sort reversal for active flow instead of stagnant flow with the MOMA system.
3. The MICHI neuroprotection system is a regulatable flow reversal (high-flow)
Advantages and Disadvantages of Brain Proximal Protection
Advantages
1. The most important advantage is complete brain protection all the time because you cross the lesion already in full protection.
2. Tight, soft plaques, tortuous ICA (with no landing zone) are very important subsets of lesions that may require proximal protection.
3. Any guidewire may be used to cross the lesion
Disadvantages
1. As with single balloons, blood flow interruption tolerance is quite low.
2. No angio guidance, so you should use landmarks
3. Potential ECA/CCA spasm/dissection
4. Relatively contraindicated in CCA+ICA or ECA+ICA stenoses
5. May be difficult to position in complex anatomy
6. Large introducer size (8-9F)
This is currently used in 8-15% of CAS procedures but growing up quite fastly.
What about the efficacy?
The last two columns are referred to two studies that have been carried out with the MOMA and the Gore, with very successful results below 3% in stroke/death outcome in independent review and independent adjudication papers.
Here are examples of the most frequent indications for the use of proximal protection.
1. High risk, soft plaque like in this case. It is what we usually find into the basket at the end of the procedure.
2. Very tortuous distal ICA that makes difficult to find, if any, positioning for the filter.
Here are some results, and I come to the close of my presentation.
This comes from a very large register from Eugenio Stabile (close to me) from Mercogliano. They found the lowest composite stroke/death rate (1.38%) and also very good results in specific subgroups (as into high-surgical risks and octogenarians). So nice results and low complications in different subset of patients.
If you move a little bit from the major harder endpoints, and if you look into the micro-embolization with TCD (Transcranial Doppler) through the microembolic signals… This is a paper from our institution: FilterWire (in red) and MOMA (in green) throughout the different steps of the procedure of CAS. And you can that at any step, there is better protection with MOMA as compared to FIlterWire.
Similarly, if you take another endpoint like microembolization assessed with magnetic resonance imaging... This is a paper coming from Hambourg group. You can see that there is less number of embolization with MOMA as compared to the filter.
Live case
Operators: Prof. P. Montorsi - Dr. E. Stabile
Dr. L. Caputi (neurologist) will perform intra procedural TCD assessment
Prof. P. Montorsi:
This is a 60 year-old man, with multiple risk factors for atherosclerosis (hypertension, smokes 1 pack/day, NIDDM, sedentary, hypercholesterolemia), no previous cardiovascular or cerebral event. He was found, just because of a cardiological checkup, to have bilateral carotid disease.
This is his CT angiography in one slide, showing a severe, long, soft plaque of the proximal part of the LICA, arch type 1, with good collateralization of intracranial circulation.
The strategy is to go by the right radial, or in this case, by the right brachial artery. So we'll use the right brachial approach. It has been use in this institution for some time, with some very good results. We will use MOMA 8F system and of course, with proximal protection. We're going to show how we can incannulate the LICA going from the right arm through direct stenting with post-dilation. And we are going to use the Cristallo Idealle stent (6-9x40mm). Thank you.
Prof. P. Montorsi: Okay, here we are already in position.
This is the left mammary diagnostic catheter 5F that we think could be a nice catheter. We just stopped before the bone.
Prof. A. Cremonesi: Did you have a soft Terumo?
Prof. P. Montorsi: Yeah, I have a soft Terumo right in the CCA.
Dr. E. Stabile: Piero, do you always do this approach using a soft Terumo or sometimes you prefer to go ahead with a stiff one?
Prof. P. Montorsi: I usually use as first wire a Terumo wire. Let's take a picture of the lesion. Can you move a little bit to take the transcranial doppler away from the screen.
Here it comes.
So this is what I just told you. It's a very soft, severe stenosis. And I think it's quite a good indication for proximal protection. We have a nice ECA – straightforward. It shouldn't be too difficult to engage and to position a stiff wire quite deep inside to get the most support as we can. The only peculiarity is that the superior thyroid artery takes origin from the distal part of the CCA, so we cannot exclude this vessel. And even the second vessel of the ECA, probably the lingual artery, is quite close to the bifurcation. So we are going to leave two important collaterals open. But we have no other option to do because of the anatomy.
Prof. G. Coppi: This is a rather unusual approach, at least for vascular surgeons. Do you have any suggestions on what kind of anatomy do you need just to have a good approach in such a way?
Prof. P. Montorsi: So this is actually number 60 consecutive patient that we, with Bovine Type 1 or 2, treat by the right radial or brachial approach. We have nice results and it now has become the first choice of approach in this case.
Prof. A. Cremonesi: Okay. That's a very technical aspect. You placed in the right radial artery, what exactly, a 6French?
Dr. E. Stabile: Is this the standard of your practice? So you always do all your carotids with this? Or you just have this for this specific patient?
Prof. P. Montorsi: Yes. Unfortunately, we have the neurologist aboard only from time to time, when we do research, some protocols, or in very difficult cases in which we believe the transcranial will give us quite crucial information.
Dr. S. Galli: Now we go to the roadmap, Piero?
Prof. P. Montorsi: Roadmap. Okay.
Prof. A. Cremonesi: An interesting question from the floor: If the two carotids are in some way stenosed, can you treat both during the same operating time? Or if you treat one, which kind will you start from?
Prof. P. Montorsi: We used, Alberto, to do the more severe or the symptom-related stenosis, if any symptom is present. We never did two lesion at the same time because we do not want to jeopardize the intracerebral circulation.
Prof. A. Cremonesi: Is the same wire you are using the soft Terumo?
Prof. P. Montorsi: This is the same wire.
Prof. A. Cremonesi: Okay.
Prof. P. Montorsi: Now we will need to enter the major... here it comes. Now try to slide the...
Dr. E. Stabile: The catheter is going very smoothly up.
Prof. P. Montorsi: Of course. So take the roadmap off and look a little bit higher. Okay.
Dr. S. Galli: Okay, perfect.
Dr. E. Stabile: Do you prefer to go as high as you can with your diagnostic catheter so you will have better support?
Prof. P. Montorsi: Yes. Because when there is some risk to have a friction with passage of sheath or MOMA, and you need a strong support, the deeper your wire is, the better support you have.
Dr. E. Stabile: And especially in a patient like this one that is asymptomatic, we have to be reminded that we are facing always the non-believer in the carotid revascularization.
Prof. A. Cremonesi: You said that you would like to use the Cristallo, which is a stent, a true 5F crossing profile. I think that I would go through without any predilation. But in the meantime, there is an interesting question once again from the web. What about the use of Piton guiding catheter when we use MOMA? I think we have to turn this question to Gioachino. Gioachino, tell us what do you think.
Prof. P. Montorsi: In the meantime, we try to bring the MOMA system below the bifurcation.
Prof. G. Coppi: Usually for the Bovine arch, the MOMA system is quite useful for the approach from the groin, of course. As a surgeon, we perform usually approach from the groin. We are less used from the brachial or the radial.
Dr. E. Stabile: I think it's easier than I thought.
Prof. P. Montorsi: And I can tell you, Eugenio, that the Type 1, as in this case, is less favorable. It's much easier with the Type 2, when the common takes origin distal from the innominate. It's quite easy. It's even worrier than in this this case.
Prof. G. Coppi: I think it could be very useful when you have a problem of the approach from the groin.
Prof. P. Montorsi: Not always, Gioachino. If you have a very diseased aortic arch, you don't want to navigate through it.
Prof. G. Coppi: It is what we are saying -- that is an important topic point. You have to check with the CT the arch you are facing before you approach the internal carotid artery.
Prof. P. Montorsi: Okay, let's make a check.
Dr. S. Galli: We'll dilate a little more?
Prof. P. Montorsi: Okay. You can close, I think.
Dr. E. Stabile: It can be that the distal part of the varices is in one of the branches of the external.
Prof. P. Montorsi: Yeah, probably it is.
Dr. E. Stabile: I think that you have room enough to pull down the distal balloon a little bit and then inflate it.
Dr. S. Galli: Okay. Now we inflated the external.
Prof. P. Montorsi: Can we check the position?
Dr. E. Stabile: Maybe a little bit down?
Dr. S. Galli: Yeah.
Prof. G. Coppi: Piero?
Prof. P. Montorsi: Yes?
Prof. G. Coppi: What's the guidewire you are using for a good support for MOMA?
Prof. P. Montorsi: This is the Supra Core.
Prof. G. Coppi: [Inaudible simultaneous speech]
Dr. E. Stabile: Can you see the distal part?
Prof. P. Montorsi: Now we check. We make an angio check to be sure that the external is completely occluded.
Dr. S. Galli: It's good.
Prof. P. Montorsi: That's good. The other two, I just told you that it should have been impossible to exclude all the collaterals. But however, the patency of the collateral is not a really critical issue nowadays, as we are not sure if they will make a risk of embolization a true issue. We never saw it in our experience, even if a large patent superior thyroid artery. So we can take the wire out. Here it is. Okay.
So now, we decided for predilation with balloon or direct stenting.
Dr. S. Galli: We'll choose predilation?
Prof. P. Montorsi: You are the guest, so you have to decide.
Dr. E. Stabile: For me, it's predilation. I'm not sure if it's necessary, but I just don't want to be in a situation which you have some trouble in crossing with your stent.
Prof. P. Montorsi: 3-5x30mm would be right?
Dr. E. Stabile: 3-5x20mm? 4x20mm is going to be fine.
Prof. P. Montorsi: 4x20mm.
Prof. G. Coppi: I have a question for Alberto. When do you suggest to predilate?
Prof. A. Cremonesi: In very tight and calcified lesions where you can never go through the resistance during the stent placement, in order to prevent the stent misplacement mostly.
Prof. P. Montorsi: So we are going to use the Cristallo Ideale 7-10x40mm.
Quite good. So we are going to cross the lesion.
Dr. E. Stabile: Okay. So are we seeing any microembolic signals?
Dr. L. Caputi: No. We just saw the reduction of the flow.
Dr. E. Stabile: ...only the flow reduction.
Prof. P. Montorsi: Can you focus now the camera on the doppler? I'm crossing the lesion under total protection with the wire. You can see how the wire straightens up the artery. There is no bend. I made also a dilatation a little bit down to be sure to get all the lesion. Here it is.
Dr. E. Stabile: The patient is doing fine.
Prof. P. Montorsi: The back pressure is still over 40mmHg. As Eugenio taught us, that anything greater than 40mmHg should be tolerant.
Dr. E. Stabile: They should. But we cannot rest because even if we say too much, then even those ones with a pressure that are higher than 40mmHg can become intolerant.
Prof. A. Cremonesi: Piero, there is another question from the web. In which way do you choose the size of the stent: visual basis or the measurement that you did in the previous diagnostic work up, and/or QCA?
Prof. P. Montorsi: The second one is correct. We used to choose the size of the stent according to the distal common diameter. Any value below 8mm means that we can use, for example, an equal or less than 7mm stent. Anything greater than 8mm, we go for a 9mm or 10mm.
Prof. G. Coppi: And the measurement is done using echo or CT?
Prof. P. Montorsi: We're using CT angiography. We ask the radiologist to take the measurement, more or less, 1.5cm below the bifurcation.
So we are through. Can you zoom so we can see the different parts of the stent? If we will be able to do that. We need a little bit higher. Right there. Eugenio, would you help me with this position?
Dr. E. Stabile: I cannot see clearly the transition, but it should be there.
Prof. P. Montorsi: We should take into consideration when we take the wire off, we will go back to the bend of the vessels. So it’s not so bad to be little bit higher. Okay.
That's fine. Run some stent, then you can be released more easily and quickly. With the Cristallo, you need to...
Dr. E. Stabile: It really depends on the bends -- the number of bends that you have on your track to the lesion.
... And even the cost is actually the same.
Prof. P. Montorsi: So we are going to inflate the balloon.
Prof. G. Coppi: Which size?
Prof. P. Montorsi: It's a 5.5mm. In 99% of the cases we use a 5.5mm. It's more that come closer to the actual valve diameters. So we can go down. Okay, slowly go down as Gioachino told us, just to avoid prolapse of the plaque.
Now we are going to start the aspiration phase. So what does the neurologist say about the post-dilation? Any embolic signals?
Dr. L. Caputi: Not so much. I would say after the release of the stent, there were some signals that were visible here, but without shower or without curtain pattern...
Prof. P. Montorsi: It was gas seen. It was gas that was embolized, not solid. I'm sure.
Dr. E. Stabile: This means I didn't flush well the stent?
[Laughter]
Dr. L. Caputi: It was not a great reduction in the MCA flow. That was nice.
Prof. G. Coppi: Is that the first syringe, Eugenio?
Dr. E. Stabile: We're going to check the first one.
Prof. P. Montorsi: The intolerance with the MOMA is a very rare but a quite important issue.
Dr. E. Stabile: The first one, we have a good catch, with four pieces.
Prof. G. Coppi: Okay, fantastico.
Dr. E. Stabile: So you see here at the bottom.
Prof. G. Coppi: It's okay.
Dr. E. Stabile: We are going to see the other ones. The second one is already clean. Nothing in this one. I would even do another in a couple of times.
Okay, so the last one is clean.
Prof. A. Cremonesi: This is a very soft emboligenic plaque. It is through that that the patient was asymptomatic from a neurological standpoint. But honestly, looking at the piece which was caught in this procedure, personally, I think that the idea of Gioachino, which is applying a concept, which is a surgical concept... We flush, in complete occlusion of the internal, in order to remove all the debris produced.
Prof. P. Montorsi: For the posterior, is that the correct pressure, Gioachino?
Dr. S. Galli: We slide two balloons...
Prof. P. Montorsi: So we deflated two balloons.
Prof. G. Coppi: Try to inject a small amount of contrast.
Prof. P. Montorsi: External? And the common?
Prof. G. Coppi: Yes. You have to deflate the common.
Dr. E. Stabile: The aim is to flush the proximal part of the stent? where there is no lesion?
Prof. G. Coppi: Try to inject just to see if you have already diversion of flow.
Prof. P. Montorsi: Inject a small contrast.
Dr. E. Stabile: You want to aspirate an extra syringe?
Prof. P. Montorsi: So, radial or brachial? It depends on the size of the stent that we are going to use. Using the Cristallo Ideale, a one-size-fits-all, you can go with the 8F MOMA even from the radial.
Dr. E. Stabile: Piero, which kind of anti-coagulation did you use?
Prof. P. Montorsi: Double anti-platelets. You can stop the bivalirudin. Bivalirudin is an intra-procedural...
Dr. E. Stabile: When are you going to remove your sheath?
Prof. P. Montorsi: More or less one hour after the procedure, if there is no complaint from the patient.
Dr. E. Stabile: Your patient will stay here, or will go to the ward?
Prof. P. Montorsi: Stay here just for an hour, and then to the recovery room.
Prof. G. Coppi: Piero, bivalirudin is your preferred anti-coagulant therapy?
Prof. P. Montorsi: Yes, only with brachial, because the reversal of the anti-coagulation is quite predictable. And if you use a classic bolus plus infusion, within one hour or even less, the anti-coagulant is over. You can remove the sheath and compress manually with no problem.
Dr. S. Galli: Very good result. Now we see the intracranial.
Dr. E. Stabile: It seems that there is no plaque prolapse in the stent. Sometimes the transition between the average segments can create some problems of prolapse. It's really clean here.
Prof. P. Montorsi: Okay, here it is. Quite nice, more brisk, the perfusion of the left hemisphere. Look at the venous return. It is good. Let's move to the postero-anterior view. We are always more familiar than with the lateral. Okay.
Prof. G. Coppi: Absolutely perfect.
Prof. P. Montorsi: That's fine.
Prof. G. Coppi: Congratulations.
Prof. P. Montorsi: Okay, so now we remove the wire. Sorry, first go back with the MOMA. And we used to take a new angio with the MOMA below the stent.
Prof. A. Cremonesi: The fullest portion of the stent now is seen.
Prof. P. Montorsi: That's correct.
Dr. E. Stabile: It's nice, sir.
Prof. P. Montorsi: We'll tell us, "Goodbye and thank you." And we'll leave the hospital tonight. This is not true, of course. But some time we did.
Discussion & Conclusion
Answer to chat questions
Prof. P. Montorsi: If you follow the rule to keep it simple, if you're in doubt about the patient's tolerance, we do a test 30 seconds after the occlusion. If the back pressure is fine, not too much below 40mmHg, and the patient has no symptoms, we can go on. If in doubt -- if I feel that the proximal protection is going to be the only device that I can use in this patient – I prefer to put what is called a "Safety belt technique.” It’s a filter through the lesion in occlusion, then you can open up and release the occlusion at any time because I will be more protected by the filter.
Otherwise, if this is not comfortable for me, I would go with another type of protection and try to be lucky.
Prof. A. Cremonesi: Second point: we were discussing in the morning that according to the recent subanalysis of CREST, post-dilatation may decrease the two-year risk of stenosis, but overall peri-procedural stroke seems to be higher. It means, do we really need to post-dilate our Nitinol stent always? We know that the Nitinol stent will continue to expand over time, so is it really important post-dilate it?
Dr. E. Stabile: It depends on which kind of protection you are using. If you are under proximal protection, it does not change a lot on the outcome of the patient. Especially if you're thinking about post-procedural strokes, by performing a post-procedural dilatation, not... But if you are on distal protection, you increase the risk of having some problems with your filter and plaque in the filters.
Prof. A. Cremonesi: Eugenio, you published probably the largest series single-center study about MOMA. Can you remind us your final result 30-day stroke and death?
Dr. E. Stabile: It's 1.4%.
Prof. A. Cremonesi: 1.4% overall? This is death and stroke?
Dr. E. Stabile: Overall. And they were all post-dilated. Major stroke is 0.8%.
Prof. A. Cremonesi: 0.8%. And they were all pre-dilated?
Dr. E. Stabile: They were all post-dilated.
Prof. A. Cremonesi: ...all post-dilated, sorry.
Dr. E. Stabile: The 50% were pre-dilated.
Prof. A. Cremonesi: Do you post-dilate?
Prof. P. Montorsi: Sometimes the plaque is quite -- this is an empiric comment -- is quite lipid. And you see that soon after the stent deployment, you already have got a very nice lumen because of the lower resistance of the plaque, and the vessel is not calcified, and you use a stent like a very good mesh, sometimes I do not post-dilate, because I do not want to increase the risk of embolization. But in many other cases -- the fibrotic, calcified lesion -- I usually do pre-dilation because the final post-procedure diameter has been found to be an independent predictor of re-stenosis. The smaller it is, the higher the re-stenosis rate. So if you can increase it a little bit, probably it will reduced the re-stenosis.
Dr. E. Stabile: We should also consider that the meta-analysis that is considering the post-dilation in the CREST trial, they're all doing this post-dilation with an open design itself, with the largest available free-cell area. So I'm not sure if those results can be generalized to a more modern approach as they meant to tailor it to CAS. I'm sure you will not post-dilate all these open-cell design with such large free-cell area.
Prof. A. Cremonesi: I do agree with you. Personally, I have many concerns about these sub-analyses of CREST data. Personally, I post-dilate 98% of cases. I do not post-dilate on in the case when... imagine that you release the stent and you have immediately reached the nominal diameter -- That means the true lipid plaque, I don't post-dilate. It doesn't matter. Generally, I always post-dilate. And you, Gioachino?
Prof. G. Coppi: I agree completely with you. I think if you have a very soft plaque, and you don't dilate, probably you can increase the risk. Because with the soft plaque, the stent is moving, you can have a kind of scissor effect. The plaque can enter in between the mesh. So I don't think you have a reduction of the risk. In the CREST study, I want to remind you that they used only filters, and without any exclusion criteria of the very tortuous anatomy. So I don't think we can have some... not a very reasonable data.
Prof. A. Cremonesi: Okay, we have here probably the third part - the neurologist. I really would like to ask you. We were speaking about procedural neurological events during carotid artery stenting. In this center, I know perfectly that Piero is treating any kind of lesion, any kind of patient, so you do not exclude any soft plaque.
You are checking during the procedure with transcranial doppler. What happens exactly when we go in complete occlusion? Do you have many HITS, even if we are protected? Can you tell us something?
Dr. L. Caputi: In most of the cases, we really see just a small reduction of the MCA flow ipsilateral to the lesion. In most of the cases, we don't see any kind of micro-embolization. Sometimes it can happen that even if you have a real occlusion, we can see some spontaneous MES signals that could be perhaps related to the not clear occlusion of the ECA because of the collaterals. That could be an option. Other real explanation are not so sure at this time. During the procedure, when you have the CCA occluded, you really don't have any kind of shower pattern, or any curtain pattern. Sometimes you just have a single spontaneous signals. They are not so clearly related to clinical events.
Prof. A. Cremonesi: We have other point to be discussed.
Prof. G. Coppi: Regarding the concept of Piero, that is the reason why in surgery, we perform flushing of the bifurcation of the carotid, just in case of remaining debris. It is possible to send the debris toward the external with a lower risk. And I think even the balloon in the common can have some deposit of platelets. And hence, it should be better to imitate over surgery. That is our concept. Of course we need good study in order to endorse this suggestion.
Prof. A. Cremonesi: There is a question which is quite fun. We have seen a great procedure -- carotid artery stenting. We heard also important data from research that carotid stenting is safe. But why is it not so popular at the moment? Why is it not the first-line treatment for carotid stenosis or stroke prevention? I'll leave you this question... he's the vascular surgeon so...
Prof. G. Coppi: I think there are some randomized study that can be misleading. The main reason is that there was no anatomical exclusion, and there is only one protective device use. In such a way, even in surgery, I think we can take a little many mistakes. It's like if we want to perform AAA endografting without paying any attention to the anatomy. Using filter distally to the lesion, sometimes we have to toss it in. And using filter, we have an adjunctive risk, not a reduction of risk. If you have kinking, if you have small dissection, like in a case we have performed today, we take an adjunctive risk. And in the final conclusion in the study, filters sometimes are not useful. There is no data in favor of filter. We have to select a good anatomy for filter. And in other anatomies that are not fit, we have to use different devices. This is reasonable. We need a study that is just created for this purpose.
Dr. E. Stabile: One of the reasons why carotid stenting is not so popular is because, I think, we have to do our part. We have to go and speak with the people of other specialties that it can be done safely, especially if you get the right training. If you think that it's something that can be done everywhere by everyone, that is not true. It can be done everywhere if somebody that has not gotten the proper training can ask somebody to give a help, to ask the hospital to pool the patients together, and perform the procedure, in this way building his own experience. The major criticism for that trial, I think you'll all agree, is on the fact that those were done by people that were not enough trained to do the procedures. So today we have this nice case, but it's because we all got the same training. So we are all discussing on how to do this procedure. We are all using the device for the structural part of the MOMA. The only things that we were discussing were to pre-dilate or not, which kind of stent to use -- but basically, the procedure was clear in the minds of the three of us at the same way. There was no necessity to speak before starting the procedure. This is the success for making the procedures safer. I think it's something that we should learn from the surgical experience. They do this procedure in the surgical room in this way. They already know what to do. And we have to do the same for the carotid stent. Just don't leave anything to be done at the moment. So we have to know what to do, and go in the room, and do it. In this way, we can convince the community, especially the bad community of the neurologists, that it is something that can be done. [Laughter]
We should ask our friend his opinion on when and how to treat patients that are asymptomatic. What do you think? Do you think revascularization can be performed for all the asymptomatic patients? Will you suggest that there are some patients that even if they are asymptomatic, they are at a higher risk? Do you think that we can have some tools so that we can identify them?
Dr. L. Caputi: I think that first, we should follow the guidelines, in which you also think a little more for every patient. If we follow strictly the guidelines, we shouldn't treat the asymptomatic patients. But if we follow some interesting publications, mostly by English people, that think of how the asymptomatic lesions are -- I'm talking about the asymptomatic signals during a long registration... I think some kind of lesion, for example the high-lipidic high-risk plaques -- how the internal circulation is, how the perfusion is. I think apart of the symptomatic ones, we should focus on this kind of asymptomatic patients starting with the possibility to give asymptomatic signals, and also on the type of the lesion that can be really risky for these patients. This can be done by both specialists -- the interventional ones (cardiologists and neuroradiologists) and by neurologists. We have to reduce the norm in the risk that an asymptomatic lesion has to at least 2-3%.
Dr. E. Stabile: Basically what you are saying is that we just calling a different subset of patients with the same name, but they are not the same.
Dr. L. Caputi: Yes, you're right.
Dr. E. Stabile: So we consider them asymptomatic, but they're not equal.
Dr. L. Caputi: Asymptomatic that have no symptoms is, I think, too much easy. We should study these patients more than they are. And the cardiologists, you taught us how to do that.
Prof. G. Coppi: I am a vascular surgeon. I have a question for my cardiologist friends. I see all the randomized study and also now, I see many cardiologists perform CAS without any CT. What do you think about it?
Dr. S. Galli: I think that now -- not only for the interventional cardiologist or the neuroradiologist or surgeon -- I think that now, it's not possible to go and treat the lesion only with the echo doppler. I think it is important to have the second-level images. I prefer CT scan, others perform angio, but it's crucial to approach the type of lesion, to vessel anatomy and morphology of plaque, plaque composition. I think that is very important and it was discussed during the case this morning to have a second level of imaging.
Prof. G. Coppi: Of course. But angio is not enough. You can't see plaques. You can't see calcifications.
Dr. S. Galli: Absolutely. We know the characteristic before intervention when we are inside the patient.
Prof. A. Cremonesi: There is an important question about this point. Do we think that there is an adjunctive role or added value related to intra-vascular ultrasound or CT evaluation? Or even a more specific question, do we use FFR, a functional evaluation of carotid stenosis?
Dr. E. Stabile: Intravascular imaging -- I don't think it's useful for the daily practice. You can perform 99% of your procedures without using those device. That will not add too much to the value of your procedure. But sometimes when you have a doubt, when you see some plaque prolapse, and you want to decide if you want to place another stent, or if you want to go ahead and perform another post-dilation, this can be useful. And maybe with your CT, it's even easier -- the plaque parts are easier to be seen -- than with the IVUS. In terms of FFR, it could have been the aim of our procedure. Finally, there are some data that come into the literature in which people are showing that a carotid stenosis can reduce the blood flow to the brain. So far, we have always treated the carotid stenosis because we were preventing stroke, and we wanted to avoid embolization in the future of the patient. And now we are having data, maybe from the perfusion imaging of the new CT scans, in which we can see that these patients sometimes have a reduced blood flow. And this blood flow to the brain can be improved by revascularization. And together with this thing of improving the blood flow, it goes with the cognitive function of these patients. So I can tell you that there are a large number of researchers that are working on this and trying to get money from the Italian Ministry of Health, from the European community, to come and to prove this concept to us. If we will be able to prove that we can treat the carotid stenosis because it has impaired the blood flow and the function of the brain, then our indication will change completely in the field. And this will go to the FFR in the end. But first we need to prove that we can do something because there's a flow impairment. If we have this indication then there's a sense to use the FFR to prove that the carotid stenosis is impairing the flow.
Prof. A. Cremonesi: Some points on the stent now. We have two questions. The first one is on open-cell and closed-cell. And is there any role for drug-eluting stents in carotid?
Prof. P. Montorsi: That's a good question. So open-cell, closed-cell, whatsoever -- we still follow the institutional recommendation or guideline -- that is to use closed-cell in patients with a lipid plaque or soft plaque, and open cell in very fibrotic or calcified lesion. We had very nice results using this recommendation or using this strategy.
Drug-Eluting stent or drug-eluting balloon: We published an experience with drug-eluting balloon for instant re-stenoses. And we have only of course 8 cases because unfortunately the re-stenosis rate is so low. However, the result was quite good up to 3 years follow up. No one re-stenosed and they were all aggressive re-stenoses at the time it was discovered at a mean of 8 months after the index procedure. So this result opened up another possibility of the use of a drug-eluting balloon, also from the periphery, as Eugene has shown in a last published paper, and also in the carotid. The results are quite good, so this is going to be probably a new indication for the drug-eluting balloon.
Prof. A. Cremonesi: But I think, personally, that if I had to create an instant re-stenosis, probably today, the best solution could be the drug-eluting balloon. I mean, it's an extrapolation, obviously, of what we know from coronary side... And now from some initial data from peripheral side. But actually, I would use it.
Another good point: Who is using the Delphi Consensus for planning the procedure?
Dr. E. Stabile: I'm not.
Prof. P. Montorsi: I'm not.
Prof. G. Coppi: What about it?
Prof. A. Cremonesi: What about it? That's a great point! Great answer. [Laughter]
No, I mean, I know perfectly the Delphi Consensus for the reason that I was in the panel for deciding if it was interesting or not. Actually, it's a grading system based on the plaque anatomy, symptoms, mostly the aortic arch configuration (elongation, tortuosity), in order to define if a procedure will be straightforward or very, very complex. It is obvious that, personally, I think it can be a nice solution for beginners. If you want to understand exactly, based on the expert panel, what can be really a complex procedure, please go toward the Delphi Consensus. Obviously, I am here... probably one of the team...
Dr. E. Stabile: I think we are all using the Delphi Consensus, we are just not making the numbers.
Prof. A. Cremonesi: Exactly!
Dr. E. Stabile: Because the Delphi Consensus was a way in which the experience of large volume operators was translated into a paper that could be understandable for all the readers. But at the end of the day, we are all using the Delphi Consensus. That is only the way to transmit your large experience to somebody that is starting, to make him understand that before approaching a carotid stenosis, there are some things to be considered.
Prof. G. Coppi: There is an important point against CAS -- that is the possible dementia in the long term due to the microembolizations. I want to tell you our recent experience using the markers of brain damage during CAS. Surprisingly, we have more damage during open surgery versus CAS. We were rather surprised, but it is a real data.
Dr. E. Stabile: Which markers did you use? The SB100?
Prof. G. Coppi: No, the specific markers for neural damage.
Dr. E. Stabile: The ones detectable on the serum?
Prof. G. Coppi: Yeah.
Dr. E. Stabile: Yeah, the SB100.
Prof. G. Coppi: That is interesting. But the reason could be that during open surgery, we have a very long clamping of the carotid. I mean, not 5 minutes or 3 minutes, but 30-50 minutes. And for now our neurology, there is a chance of possible damage of a small area of brain that you can detect at the beginning even with MRI. So, I think we have to open a window on this problem.
Dr. E. Stabile: Unfortunately, there are no data on the cognitive function of the patient after the two procedures. It would be nice -- now that we have the CREST trial, we have a five-year data -- It would be nice to check the cognitive function of both the patient subgroup and see if there was a damage in the long-term.
Prof. P. Montorsi: Can I just make a comment for our audience? Is it still valid, using proximal protection, that the faster is better (referring to the occlusion time)? Or take your time if the patient is tolerant and you can do every step? "Go slow, finish first," as someone says.
Prof. G. Coppi: As a vascular surgeon, we had the same problem some decades ago. And we have learned that we have to go, not slowly, but just safe; not to go so fast and make some mistakes.
Prof. P. Montorsi: So the middle state virtue as many said.
Prof. G. Coppi: Exactly.
Dr. L. Caputi: If I just can say something about this one -- about your question. When we usually do the carotid balloon occlusion test for patients who have aneurysms, we need to stay in occlusion for more than 40 minutes. And we see everything by the angiogram, by the doppler, by other neurophysiological test. I would say, if there is real compensation even with low general pressure, the patient should not have any kind of...
Prof. P. Montorsi: However, these are normal patients.
Dr. L. Caputi: Hmm, I would say normal, but...
Prof. P. Montorsi: ...young patients, the artery is normal, AV malformation, whatsoever. I looked with many neighbor neuroradiologist as they put the catheter quickly up in the carotid artery that are very smooth artery, nice and normal. It’s completely stuffed in an 80 year-old man with a significant stenosis. So microcirculation is gone...
Dr. L. Caputi: I would say don't be afraid to be as fast as possible.
Prof. P. Montorsi: That's correct.
Prof. G. Coppi: Two or three minutes more is not a real risk.
Prof. P. Montorsi: Yes.
Dr. L. Caputi: Absolutely.
Prof. A. Cremonesi: There is another burning point. We spoke about indication and patient selection. Now, contraindication. A very honest overview for contraindication to carotid artery stenting. I really would like to know what your opinion is about true contraindications. In my hospital, I have to disclose very honestly that we refer a patient to a vascular surgeon not more than in 2% of cases. So it means that actually we do everything. I don't know. We, obviously, as a panel of expert are spoiled by our experience, for sure. But do we really think that there is a true contraindication to carotid artery stenting today, with the devices and with the experience we have?
Dr. E. Stabile: One thing could be if the patient cannot take dual anti-platelet therapy.
Prof. A. Cremonesi: Obviously.
Dr. E. Stabile: And the other thing is inexperience.
Prof. A. Cremonesi: So one is a point of the patient, and the other one is the operator. Okay, so the contraindication is the operator. [Laughter]
Dr. E. Stabile: If you are in your learning curve, you have to consider the tough cases. You can ask the surgeon to solve the issues for you.
Prof. G. Coppi: Perfect.
Dr. E. Stabile: That's meanwhile that you build your experience.
Prof. A. Cremonesi: So self-assessment is very important.
Dr. E. Stabile: It's crucial.
Dr. S. Galli: I think that there is a real part we've seen, Eugenio. I think that it is very important to know the very difficult arch. And when you think that surgery is better and less risky than the intervention. Indeed, there is self-assessment. And the other point is contraindication but also is no indication. For example, a poor patient with a tight lesion, with low expectancy of life, or very poor... it's a no risk.
Prof. P. Montorsi: Yes. I think that poor cerebral condition is the major contraindication for any type of revascularization. If you go more deep into the anatomic, I would stay away from heavily calcified lesions, 360 degrees, diffused, very bad, both for the common and the targeted bifurcation, and very, very difficult tortuous vessels, especially in asymptomatic older patients. Just stay away.
Prof. G. Coppi: I agree completely with Piero -- that calcification of the common, the arch of the common, and also ring calcification of the internal carotid artery -- that is the anatomical contraindication. We prefer the open surgery for the very young people, because at the moment, we have experienced 5-10 years of CAS but not of 20 and 30 years as we have for open surgery. In a very population, the first option for us is open surgery. But if the patient prefers CAS, of course, we don't refuse.
Prof. A. Cremonesi: Thrombus-containing lesions?
Prof. G. Coppi: No, it's not a problem with proximal protection.
Prof. A. Cremonesi: So it means that...
Prof. G. Coppi: Even in acute patients
Prof. A. Cremonesi: Even in acute. Because now we can really move from the so called "stable" patient, even if symptomatic, through acute carotid syndromes. You are performing acute carotid syndromes?
Prof. G. Coppi: Yeah, we are doing it. I think that this is an important point because there is a suggestion to be able to perform the procedure in 20 or 40 minutes. But with CAS, it's possible. With surgery, it takes more time. It's much more difficult to perform staying in a very short period of time. It's more heavy for surgeons. In 40 minutes, we can do everything and go home in peace, while with open surgery, it can take 2-3 hours and it takes more time. It's more heavy for the patients. And generally speaking, they are, in a vast majority of cases, very elderly. And the evidence is for our patients is 76-78. So I think for these patients that was contraindicated in CAS, we have similar results if the anatomy is suitable than in open surgery.
Prof. A. Cremonesi: If I comprehend correctly, any kind of proximal protection, (because we are speaking about MOMA but in the past we have also other devices), changed consistently our way of approaching carotid lesions for a meaningful objective of stroke prevention. Our vision is really wider at the moment, if I understand correctly
Prof. P. Montorsi: I think that if you... the way you use proximal protection... I feel very comfortable with the device and it makes me more relaxed and calm during the procedure because I think this is the best way to go. What I would like to say, if I could spend a word for proximal protection, is -- just not as the case as we just did some time ago -- Don't use proximal protection only going from the groin or the femoral, but expand the indication encompassing different types of lesion, types of variance, different types of anatomy. I just showed you that you can go from the right radial or right brachial approach, or even from the left. And there is no reason why you should have more complication, bleeding, or unsuccessful procedure. So this opens up to a larger patient that you could use this type of protection. And if you use the 8French, so you reduce the ?? So you reduce [inaudible] as compared to the Gore diameter, you can go very successfully from the brachial and you can get very good results. So we need proximal protection to be used even in more complex anatomy, probably with controlled randomized trials with some subclinical endpoint to see whether you can reduce the time, the radiation... and you get also a very good clinical result.
Dr. E. Stabile: But do you suggest to use the brachial or radial approach only for the Bovine arch?
Prof. P. Montorsi: Bovine arch is the classical indication.
Dr. E. Stabile: But you won't expand to all of them.
Prof. P. Montorsi: That's correct.
Prof. G. Coppi: I have a question again for you interventional cardiologists. In STEMI, in acute you are using the Ticaglerol, I suppose, while we have to use still Plavix in acute patients? We know that it's active in almost one day. So why not should we use Ticaglerol also in acute patients for CAS?
Dr. S. Galli: Probably the only indication... we have no experience in the peripheral... but probably one indication is if you perform acute CAS. Because 90% of the cases is elective and you choose... If the patient is not prepared very well, this is an option. Another point is if you use a new agent like Ticaglerol or Prasugrel. This is a very important point in very high-risk lesions.
Prof. A. Cremonesi: At least the resistance, we know perfectly in the 20-25% of patients that Clopidogrel should be overcome. Anyway, it's an important point, but nothing from the science, unfortunately.
About science, what are the ongoing trials about CAS? Have we something really ongoing which will clarify in some ways the never ending debate between carotid artery stenting and carotid endarterectomy? Something ongoing?
Dr. E. Stabile: One is the ACST-2, in which they are trying to enroll patients from high volume centers, both from endarterectomy and from carotid stenting. And we hope that the outcome of this trial can be more reliable than the trials that we got so far. And this is mainly for the symptomatic ones.
For the asymptomatic, we are still waiting for the NIH in US to support the CREST-2 trial. The CREST-2 is going to analyze asymptomatic patients, best medical available therapy to CAS, and see really what is going to be the outcome of these patients. As you know, now the people that are in favor of the medical therapy are claiming that there is 0.5% stroke risk for asymptomatic patients, and this is making any kind of revascularization too challenging. These are the main two, I think, in my opinion. I don't know if you know something ongoing.
Prof. A. Cremonesi: Probably it would really be very nice to have a great randomized trial between proximal protected carotid stenting and carotid endarterectomy, which in my mind could really be the nice next randomized trial. But unfortunately, no funding is available at the moment.
Prof. P. Montorsi: No more money.
Prof. A. Cremonesi: But Eugenio, you touched the good point in the best medical therapy, and there was a pending question: What is the role of aggressive statin therapy in order to stabilize the plaque or the patient in some ways? Is there any important...
Dr. E. Stabile: We learn from the SPARCL trial, in which they were taking even patients that already had a stroke with a carotid stenosis, and they were given Atorvastatin 80mg per day, the stroke risk was reduced by 30%. One year of stroke risk was reduced by 30%. Not even increase in the intracerebral hemorrhage -- That was a classical pitfall of the statin -- because this was common only in those patients who had a stroke due to an intracerebral hemorrhage. So for sure the high-dose statin can help in preventing the stroke risk in these patients. I don't know if you agree.
Dr. L. Caputi: We have the people that had a stroke this Atorvastatin 80mg. For the people that had to perform elective, let's say, carotid stenting, we usually see 20 or 40mg.
Prof. G. Coppi: What is interesting is that there is a study that demonstrated that at one year, not more than 50% of the patients are following the therapy. That's the medical therapy. I thought that randomized study is important, but the real life is sometimes different.
Regarding the ongoing randomized studies, I think that if we have not a study including a previous good study of the plaque and the anatomy, I think they are not all right. I think only in the CREST-2, it's included previous CT.
Prof. P. Montorsi: Can I make a comment. If you just, for a moment, go through our experience of almost 1000 procedures, 78% of the patients were not on target when started. They entered the hospital not on target. It's quite a frequent finding in coronary artery disease.
Dr. E. Stabile: I have even worse data. If you consider, we are collecting the medical therapy of the patients that are referred to us, as a tertiary center for the treatment of carotid stenosis. We insisted that the things to have are aspirin, second anti-platelet agent, ACE inhibitors, and statins. Only 25% of them are taking the four things. And they're are asking to be treated for the CAS.
[Laughter]
So it means that everyone that has seen them has recognized that there's serious risk factor for atherosclerosis, and they're not even getting the therapy. So I think we all have to make an effort. If we really want to follow, let's say, the European guidelines... If we really want to reduce the burden of cardiovascular disease, we need to follow all these guidelines altogether.
Prof. P. Montorsi: So when talking about best medical treatment, I used to talk about best medical treatment plus interventional procedure. This area, I really have much to do to be more successful in this.
Prof. A. Cremonesi: Another good point: Combine disease carotid and coronary -- What do you do in this high-risk subset of patients? What to do first? Timing is very important. Relationship between, for example, of surgical and endovascular options.
Dr. S. Galli: I think that the real problem is if the coronary is a surgical indication. Because if there's really a percutaneous indication, we perform normally a coronary before and then complete with carotid. The problem is for the surgical, for the extracorporeal… I think that the best way is perform before a percutaneous, a carotid, and then surgery.
Prof. G. Coppi: With open surgery, it should be difficult to treat patients with the double anti-platelet therapy. Some are treating patients. Some cardiac surgeons are refusing this kind of patient.
Dr. S. Galli: Yeah. But if you have a very tight lesion, sometimes there is a problem during the circulation, so it's not low.
Prof. A. Cremonesi: So it means we can make a scenario. Imagine that you have an 80% symptomatic carotid stenosis, and the left main is asymptomatic. What should be done?
Prof. P. Montorsi: Left main.
Prof. A. Cremonesi: Yes. Great. Generally, in our institution, when we receive this kind of patient, generally we do them in a single stage. We go from the lab to the cardiac operating theater. Otherwise, the opposite means from the operating theater. But just in a single setting. That's what we try to do. It's not an easy organization because we have to put everything together. The great option should be the hybrid endo-suite. I start, for example...
If we have to treat with a left main PCI, what's first and what's second?
Prof. P. Montorsi: I used to go first with where the symptoms are present, either the cerebral or the heart -- that will guide the procedure.
Dr. L. Caputi: If you have a symptomatic carotid and you're treating the heart, you have both risk -- hemodynamic and embolic risk.
Prof. P. Montorsi: We should take into consideration that symptomatic patients for carotid artery disease do have 3-vessel disease in almost 25% of the cases. So we need to check for it and then stratify the risk. Sometimes the asymptomatic stenosis, with no history of coronary disease, passing by we have to look first at the coronary circulation, and sometimes we stop because it was 90% proximally stenosed with an asymptomatic stenosis. We do first the coronary circulation in patients with asymptomatic in both territories. In that case, I would say, cerebral can wait. Do first the coronary circulation.
Dr. L. Caputi: Yeah, because the reduced cerebral perfusion could be also depending on the heart, even in both asymptomatic patients.
Prof. G. Coppi: Is it not a problem for cardio-surgeons to treat patients under double anti-platelet therapy?
Prof. P. Montorsi: Of course it's a problem.
Prof. G. Coppi: What's the difference in bleeding?
Dr. E. Stabile: It shouldn't be a problem because all the available data on cardio-surgery, we do with anti-platelet therapy much better than without. It's not in the real life, but it shouldn't be. I'm sure you're reminded of the study that Francesco Versace did on the hybrid thing, in which they were doing the carotid intervention the first thing, and they were using only aspirin and heparin. In the afternoon, they were doing the CABG, and then they would start the process...
Prof. G. Coppi: It should be an option for open surgery in this kind of patients.
Dr. E. Stabile: I don't see why not.
Prof. P. Montorsi: There is nothing against it.
Dr. E. Stabile: Really, I don't see why not do it. We are coming from a long history in which the surgeons, they were doing both coronary bypass and carotid; so I don't see why not now. I really don't see why now it should be different. Just to do a carotid stenting, I don't think it takes any advantage on that one.
Prof. A. Cremonesi: Another important scenario proposed by the web: Imagine that we have a patient with a stroke, and we study the patient and we see that there is an important tight stenosis obviously omolateral to the hemispheric lesion. When do you perform carotid artery stenting? How long do we have to wait for the intervention?
Dr. L. Caputi: Following the treatment guidelines, the guidelines say that the TEA -- the revascularization -- should be at least after 2 weeks to get the 90% benefit from the procedure. Nothing is really written in the guidelines about the acute treatments, but I would follow what you were saying before that we should at least try to compare a proximal protection with the TEA in order to prevent acutely a second event. Up to now, two weeks from the event for the TEA. But some centers as yours, they do it in more than 24 hours.
Dr. E. Stabile: Can you help me to understand why you have to wait two weeks?
Dr. L. Caputi: Because they say there is more bleeding. And because it's risky for the type of the plaque because it's really unstable. And also because if you have to operate on the patient, you can have some kind of complications depending on the operating set.
Prof. G. Coppi: In our center, we are always doing a perfusion CT. In case we have a large penumbra and more damage, we do immediate treatment. And in case we have a large area of dead brain, we of course postpone the procedure for 2 weeks.
Prof. A. Cremonesi: But I have a question for the neurologist. We are speaking of minor stroke. And if you have a really major stroke -- a significant major stroke -- is it the same situation?
Dr. L. Caputi: I would say that the minor stroke, like even in TIAs, can hide an immediate major stroke. So for us, it's a similar thing. It's an event, and so we have to treat following the guidelines, or in big centers as yours, try to study as best as possible the patient. If you have a major stroke and the risk of a huge revascularization is high, you have to wait for it. Otherwise you will have a risk of hemorrhage. But I would say if you have a symptomatic carotid, and you have a major stroke, anyway you have to treat him because... If you want to reduce, you can wait for a week, 10 days, and you operate within 2 weeks.
Dr. S. Galli: I think a good rule is that in a very, very acute phase, to have time to perform double anti-platelet therapy and statin to stabilize the plaque. Then no more than one month.
Prof. G. Coppi: It depends on the time when the patient is arriving. If he's coming 1 or 2 hours just after the symptoms, we do the perfusion CT. We work together with the neuroradiologist and we perform PTA stenting of carotid. And then we try to recuperate the major cerebral artery using the Solitaire, or Trevor, or other devices like this.
Prof. A. Cremonesi: But just to explain exactly what the penumbra is -- you spoke about penumbra.
Dr. L. Caputi: It's a part of the brain that is not dead. So you try to... It's like it's hibernated. It's like a "stunned" part of the brain that can be restored by an acute treatment.
Prof. A. Cremonesi: It's a viable part of the brain which is surrounding the infarct zone.
Dr. L. Caputi: Yes. So we have to see this mismatch between the diffusion and the perfusion.
Prof. P. Montorsi: It's what we call the in the coronary circulation "the lesion." It comes from the necrosis of the lesion and the ischemia. They are waited to be reperfused.
Dr. L. Caputi: We know this thing because it can also begin [inaudible simultaneous speech] and then we are going on.
Prof. A. Cremonesi: Good. I think that now we do not have any other questions. And I would really leave you the honor to close and wrap up this great session.
Prof. P. Montorsi: Thank you so much. We've shown to the web population 3 live cases and 3 recorded. And we'll find on the InCathLab site of patients treated with proximal protection, quite challenging lesions with very good results. I would like my first message to widen the indication to use this protection, not only in very incredible case of plaque total dissection, but also as a default technique in every case, I would say. Because my impression is that you will get better result than with any other type of protection. However, you should be, as Eugenio told before, the procedure should be in your hands. A sound experience is of paramount importance. So let's do the CAS procedure in very experience hands, in high volume centers that work with passion and with research.
Prof. A. Cremonesi: So thank you very much to all of you. Just to remind us, I really give my warm thanks to Luigi Caputi (our neurologist), Gioachino Coppi (our enemy) [laughter], Stefano Galli, Piero Montorsi, and Eugenio Stabile. Thank you for your attention. Many thanks. Bye bye.
[Applause]
------ end of transcription ------
Suggestions
San Francisco : Tuesday, March 26th 2024 from 09am to 10:30am (GMT+1)
New York : Tuesday, March 26th 2024 from 12pm to 01:30pm (GMT+1)
Buenos Aires : Tuesday, March 26th 2024 from 02pm to 03:30pm (GMT+1)
London / Dublin : Tuesday, March 26th 2024 from 05pm to 06:30pm (GMT+1)
Paris / Berlin : Tuesday, March 26th 2024 from 06pm to 07:30pm (GMT+1)
Istanbul : Tuesday, March 26th 2024 from 07pm to 08:30pm (GMT+1)
Moscou / Dubaï : Tuesday, March 26th 2024 from 09pm to 10:30pm (GMT+1)
Bangkok : Wednesday, March 27th 2024 from 12am to 01:30am (GMT+1)
Shanghai : Wednesday, March 27th 2024 from 01am to 02:30am (GMT+1)
Tokyo : Wednesday, March 27th 2024 from 02am to 03:30am (GMT+1)
Sydney : Wednesday, March 27th 2024 from 03am to 04:30am (GMT+1)
Wellington : Wednesday, March 27th 2024 from 05am to 06:30am (GMT+1)
CAS e-Contest Final Results
an interactive european contest on carotid artery stenting
San Francisco : Wednesday, February 12th 2025 from 08am to 09am (GMT+1)
New York : Wednesday, February 12th 2025 from 11am to 12pm (GMT+1)
Buenos Aires : Wednesday, February 12th 2025 from 01pm to 02pm (GMT+1)
London / Dublin : Wednesday, February 12th 2025 from 04pm to 05pm (GMT+1)
Paris / Berlin : Wednesday, February 12th 2025 from 05pm to 06pm (GMT+1)
Istanbul : Wednesday, February 12th 2025 from 06pm to 07pm (GMT+1)
Moscou / Dubaï : Wednesday, February 12th 2025 from 08pm to 09pm (GMT+1)
Bangkok : Wednesday, February 12th 2025 from 11pm to 12am (GMT+1)
Shanghai : Thursday, February 13th 2025 from 12am to 01am (GMT+1)
Tokyo : Thursday, February 13th 2025 from 01am to 02am (GMT+1)
Sydney : Thursday, February 13th 2025 from 02am to 03am (GMT+1)
Wellington : Thursday, February 13th 2025 from 04am to 05am (GMT+1)
Complex CAS handling
Roadsaver TM Insights Week: Celebrating a Decade of CAS Advances
San Francisco : Friday, February 14th 2025 from 08am to 09am (GMT+1)
New York : Friday, February 14th 2025 from 11am to 12pm (GMT+1)
Buenos Aires : Friday, February 14th 2025 from 01pm to 02pm (GMT+1)
London / Dublin : Friday, February 14th 2025 from 04pm to 05pm (GMT+1)
Paris / Berlin : Friday, February 14th 2025 from 05pm to 06pm (GMT+1)
Istanbul : Friday, February 14th 2025 from 06pm to 07pm (GMT+1)
Moscou / Dubaï : Friday, February 14th 2025 from 08pm to 09pm (GMT+1)
Bangkok : Friday, February 14th 2025 from 11pm to 12am (GMT+1)
Shanghai : Saturday, February 15th 2025 from 12am to 01am (GMT+1)
Tokyo : Saturday, February 15th 2025 from 01am to 02am (GMT+1)
Sydney : Saturday, February 15th 2025 from 02am to 03am (GMT+1)
Wellington : Saturday, February 15th 2025 from 04am to 05am (GMT+1)
CAS vascular surgeons' perspective
Roadsaver TM Insights Week: Celebrating a Decade of CAS Advances
San Francisco : Thursday, June 22nd 2023 from 09am to 10:30am (GMT+2)
New York : Thursday, June 22nd 2023 from 12pm to 01:30pm (GMT+2)
Buenos Aires : Thursday, June 22nd 2023 from 01pm to 02:30pm (GMT+2)
Reykjavik : Thursday, June 22nd 2023 from 04pm to 05:30pm (GMT+2)
London / Dublin : Thursday, June 22nd 2023 from 05pm to 06:30pm (GMT+2)
Paris / Berlin : Thursday, June 22nd 2023 from 06pm to 07:30pm (GMT+2)
Istanbul : Thursday, June 22nd 2023 from 07pm to 08:30pm (GMT+2)
Moscou / Dubaï : Thursday, June 22nd 2023 from 08pm to 09:30pm (GMT+2)
Bangkok : Thursday, June 22nd 2023 from 11pm to 12:30am (GMT+2)
Shanghai : Friday, June 23rd 2023 from 12am to 01:30am (GMT+2)
Tokyo : Friday, June 23rd 2023 from 01am to 02:30am (GMT+2)
Sydney : Friday, June 23rd 2023 from 03am to 04:30am (GMT+2)
Wellington : Friday, June 23rd 2023 from 05am to 06:30am (GMT+2)